Osteoarthritis
July 10, 2019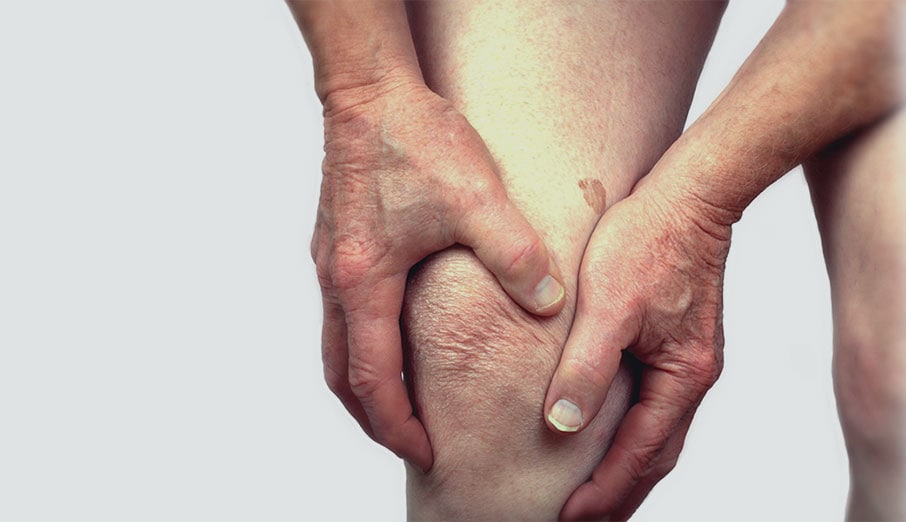
Osteoarthritis (OA) is a super common condition causing joint pain. It may effect a number of different joints in the body, but is particularly common in the fingers, thumbs, neck, back, hips and knees.
The name “osteoarthritis” can be split up into osteo (meaning bone), arthr (meaning joint) and itis (meaning inflammation). So osteoarthritis literally means inflammation of the parts of bones which are part of a joint. It is a chronic degenerative disorder, where the joint surfaces and other structures are degraded over time.
Symptoms of OA include pain, loss of joint range of motion, joint swelling and weakness. In early stages, or more mild cases of OA, pain may only occur first thing in the morning and/or following exercise.
So what happens to a joint that is osteoarthritic and how can we treat/manage it?
What is happening to the joint?
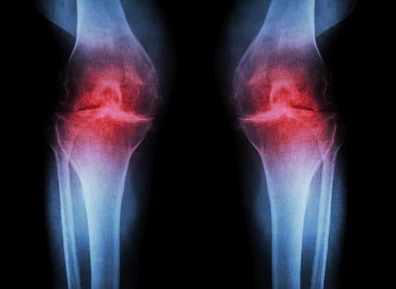
OA affects a number of different structures within a joint.
Articular cartilage
A bone’s joint surface is covered in a layer of very smooth cartilage called “articular cartilage”. When articular cartilage is healthy it allows a smooth surface to articulate with another smooth surface in order to allow more free movement in a joint. In the case of osteoarthritis, the articular cartilage begins to degrade and no longer be smooth. It may develop divots and thin portions, sometimes to the point that the underlying bone may be exposed. When you hear an OA sufferer refer to their joint being “bone on bone” this is what they are referring to.
Joint capsule
All movable joints are encapsulated by a membranous joint capsule. This joint capsule may become inflamed and irritable a joint with OA.
Subchondral bone
The portion of bone immediately below the articular cartilage can also begin to degrade and develop cysts and other lesions.
Other structures
Other structures which can be affected include ligaments and other cartilage structures (such as the menisci in the knees). Small bony outgrowths (osteophytes) may also form.
How can we treat / manage OA?
Unfortunately, OA is not something that can be cured. However it can be treated and managed to slow it’s progress, reduce associated pain, improve range of movement and strength, and therefore improve function.
Management may include techniques such as massage, joint mobilisations and electrotherapy for pain relief, increased range of motion and management of inflammation.
What’s most important for the management of OA is techniques to manage the condition yourself at home. Exercise is a big part of this, and management of OA should include exercises to strengthen specifically relevant muscles, exercises to improve general strength and aerobic capacity, and exercises to improve or maintain range of motion in affected joints.

Contrary to popular belief, exercise will not “wear out” a joint. Rather, graduated increases in weight bearing exercise actually stimulate the body to do a better job of maintaining the articular cartilage.
Weight loss is also a very important part of management of OA. There are lots of studies which show that even fairly modest reductions in weight can have a significant impact on reducing pain associated with OA of weightbearing joints (eg knee, hip, lower back).
Your GP should also be involved in the management of your OA, and they will be able to advise in terms of medications and other potential treatment options.
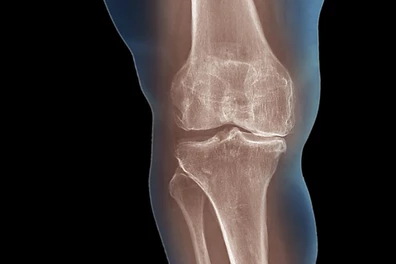
What is interesting is that the severity of OA symptoms actually correlate very poorly with the severity of OA changes which may be seen on X-rays or other imaging. Some people with no symptoms may have severe joint degeneration on an X-ray, while someone with severe OA symptoms may have very minor changes evident on an X-ray.
This means two things.
- While imaging certainly has its place, it should not be taken as the be-all-and-end-all of your condition. The pain and limitation of activity is of far more importance in determining the severity of your condition.
- As with other types of chronic pain, other factors such as your understanding of the condition, your psychological state, your past experiences etc have an influence on the pain you feel, and so management of these issues may be helpful in reducing your symptoms.
Are you suffering OA and need input to assist to manage it? See our physiotherapist in Aubin Grove today!
-
 What Can Make Neck Pain a Headache?
What Can Make Neck Pain a Headache?
Often people experiencing a headache are also experiencing neck pain/tightness a...
-
 How Physio Can Help Your Headaches
How Physio Can Help Your Headaches
Headaches are no fun. Some people will only experience short-term headaches ever...
-
 Muscle Strains
Muscle Strains
Winter sports are back and with them come more muscle strains, particularly hams...
