We Need to Rely Less on Medical Imaging for Back Pain
March 28, 2021
Medical imaging technology seems great, right? It can take pictures of what your tissues look like and tell you exactly what’s going on. Brilliant!
Well, often it is brilliant, and for a number of presentations it’s absolutely necessary. But for lower back pain in particular, it’s over-prescribed and over-relied on.
Sometimes a scan is indicated for lower back pain. For example if a fracture is suspected, or if significant neural symptoms need to be investigated. But for the vast majority of lower back pain presentations, medical imaging is not necessary.
Why isn’t medical imaging necessary in these cases? Doesn’t it show you what’s going on?
Many of the changes that show up on X-rays, CT scans, MRIs etc, are actually normal ageing-related changes that, in many instances, don’t cause pain. A substantial percentage of the pain-free population will have changes such as disc bulges, loss of disc height and facet joint degeneration, as illustrated by this graph.
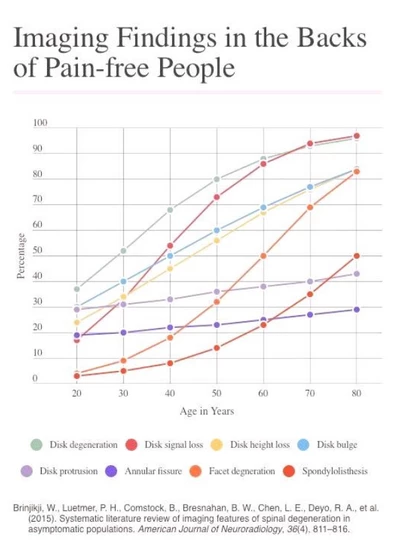
This graph might be a bit difficult to read, but it shows, for example, that “facet joint degeneration” is visible on lower back imaging in about 20% of pain-free 40 year olds, 50% of 60 year olds etc.
Because these changes are often present in people with no back pain, we can’t definitively say they are the cause in someone with back pain. Further, there are also many causes of back pain which won’t show up on a scan, and so these causes may be ignored all together if too much reliance is placed on scans.
This isn’t to suggest that there is no use in scanning people’s backs at all, but they should be used sparingly, and their findings should be interpreted in the context of patient’s particular presentation. For example, if your symptoms aren’t consistent with discogenic pain, then any changes to the disk can be taken with a grain of salt. They’re common in people with no back pain anyway!
I’m happy to pay for a scan, so what’s the harm?
The harm in placing too much reliance on scans arises in two cases of patients.
Firstly, for patients with severe symptoms, but little to no changes showing up on a scan. It’s all too common for these patients to be made to feel that they’re “making their pain up”. This might just be how the patient feels if they are putting too much stead in the scan results, or sometimes a health professional flat out tells them this!
Secondly, for patients with fairly minor symptoms, but with numerous age-related changes showing up on their scan. Someone with minor symptoms who is told they have “multi-level degenerative disc disease”, “vacuum phenomenon”, “multi-level facet joint arthropathy”, “central canal stenosis” etc will likely become more worried about their back. Their back must be worse than they thought!”
But, of course, many or all of these changes are likely not contributing to symptoms and so should be thought of as normal, age-related changes.

A recent study showed that early MRI imaging of back pain patients actually led to substantially worse outcomes for the patients in terms of recovery time, ongoing symptoms and impact on activity levels.
Recent research has found that some surprising things actually correlate more with back pain than changes on imaging. For example stress and mental health issues have a very strong correlation with back pain. So too does fear of certain movements or activities.
This research is leading us away from over-reliance on imaging. While imaging certainly still plays an important role, it’s important that we don’t see it as the be all and end all of making a diagnosis and guiding rehab.
-
 What Can Make Neck Pain a Headache?
What Can Make Neck Pain a Headache?
Often people experiencing a headache are also experiencing neck pain/tightness a...
-
 How Physio Can Help Your Headaches
How Physio Can Help Your Headaches
Headaches are no fun. Some people will only experience short-term headaches ever...
-
 Muscle Strains
Muscle Strains
Winter sports are back and with them come more muscle strains, particularly hams...
